The Importance of Quantitative Pupillometry Today and What it Will Bring in the Future

Pupillometry has been around for centuries, and it may be much older than that. Yes, really. Dating back all the way to Robert Whytt, an 18th Century Scottish Professor in theoretical medicine, who first coined the reflexive action of “sympathy” as it relates to the pupils and neurology. He even went so far to determine it was a cyst inhibiting the reflexive action in a hydrocephalic child, a condition of cerebrospinal fluid buildup. Thus, we have our first documented diagnosis of a neurological challenge using pupillometry. It’s certainly impressive that Dr. Whytt was able to recognize the importance of the pupils so early on in medicine. But where is pupillometric medical technology at today and how has modern medicine expanded on Dr. Whytt’s knowledge?
Many Haven’t Evolved Best Practices Since the 18th Century.
It’s not surprising that many adopt the philosophy of “if it’s not broken then don’t fix it” and it’s easy to see why. Pupillometry is a powerful tool outright that never needed much expansion after inception. Most all innovation has come from new protocols to conduct the test rather than improving upon the technology itself. Now we can understand why the penlight is still so popular today. It’s good enough to do very good medical work. Like fire, it gets the job done for a long while until something new is needed. Surely there isn’t some way to better implement a simple light shining in the eye and seeing what happens? This would be when Quantitative Pupillary Light Reflex (qPLR) exams, or more colloquially know as Quantitative Pupillometry, enters the picture.
qPLR is A Non-Invasive Tool to Help You See the Detail
It wasn’t until the late 20th century that pupillary testing technology started to be improved upon. Major advances in cameras and computers allowed for new inventions to expand upon the status quo of medical evaluations. The advent of qPLR by means of a hardware apparatus, instead of using a penlight, offered a new route to understanding the dynamic motion of the pupil. Research quickly expanded the neurological territory in which qPLR could be useful, and surprise, it’s a big territory. This shouldn’t shock us given how integrated of a role the PLR pathway plays within the brain itself. Even with how non-invasive the assessment is. What should impress us is the level of detail in which it provides. Nearly all neurological aberrations, injuries, and challenges represent themselves within dynamic pupillary testing. Pixel level accuracy allows clinicians to capture all the important details like latencies and hippus that otherwise would be challenging to accurately observe with the naked eye. So how do we apply that detail to modern medicine?
The Pupil Tells the Story the Brain Needs to Say – Uses in Vitals, Concussion, Neurodegeneration.
Quantitative Pupillometry is particularly important today as it provides an objective, repeatable method for evaluating and monitoring many neurological conditions. A common example being concussions which is a growing concern in many fields, including sports, military, and healthcare. Concussions can have serious long-term consequences if not detected and appropriately managed. Many research articles have indicated the utility of qPLR on this front but the most prominent, and certainly the largest study, is this one which encompassed over twenty thousand patients. Twenty thousand. This is two orders of magnitude more than any other qPLR study to date. What it outlines is that qPLR detects changes in the pupils that are indicative of a concussion and help medical professionals make timely diagnoses. More importantly it can monitor a patient’s recovery and progress over time allowing for safe return to learning and activities.
But why stop at concussion? If qPLR can see the detail in that then there must be more. You’d be correct. Not only is qPLR being actively used for addiction recovery and drug assessments, but it’s going further into modern neurological challenges that have increased in prevalence. These include neurodegenerative diseases such as Alzheimer’s and Parkinson’s disease, early diagnosis of autism spectrum disorder, and even multiple sclerosis.
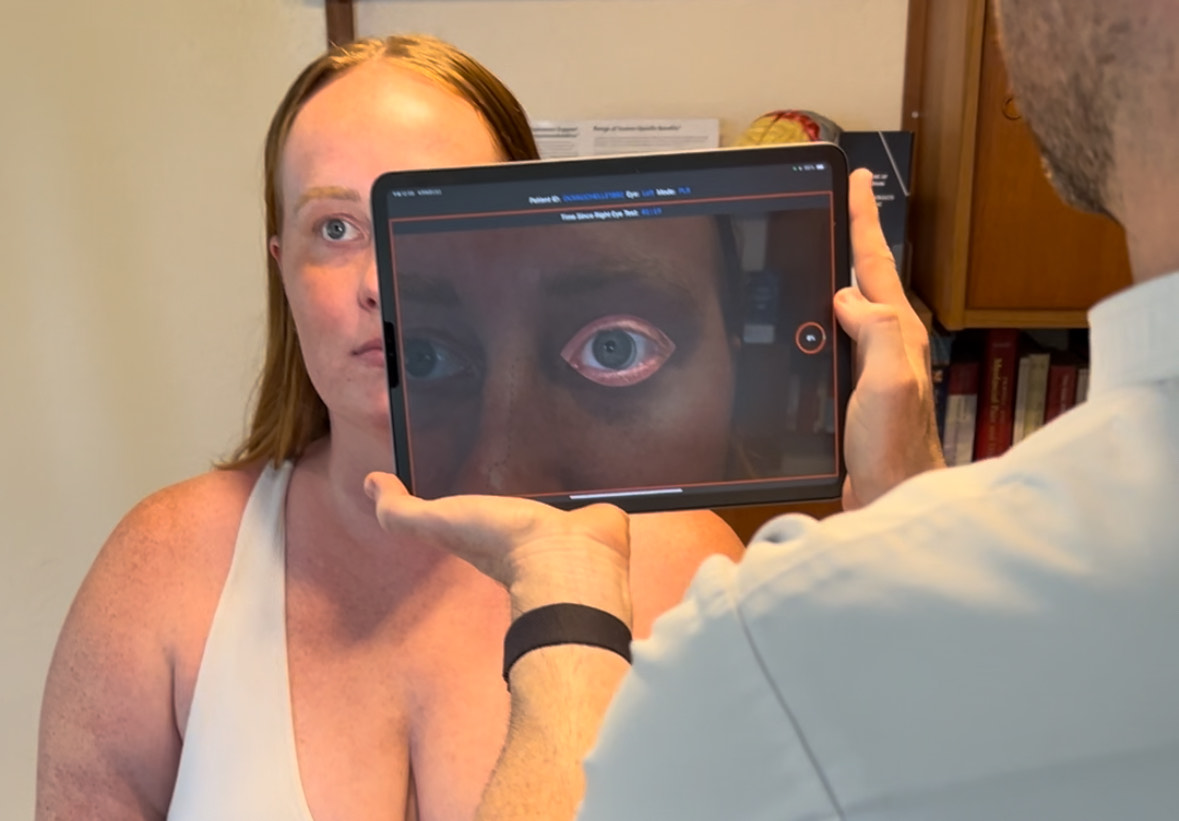
With that current landscape, could you guess what qPLR is mostly used for today? Vitals. But not in the traditional sense. Waves of clinicians are adopting new practices that better encompass the neurological system’s objective status that far surpass the narrow, commonly accepted, vitals. A simple five second test using a smartphone or tablet can now capture detailed vital neurological data to be relied upon during regular evaluations. That’s the true importance of modern qPLR in the clinic today; a broad neuro vital that tells the story of whatever the brain needs to say.
The Future of qPLR is in the Hands of the Patients
Now that clinicians and modern medicine have caught on it’s time to ask the question: What if we got qPLR vitals data whenever we needed it and not just at the clinic? Advances in telemedicine and telehealth have provided an easy access route for smartphone tests to be conducted at home. Enabling patients to provide data more consistently to their caretakers outside of the office at all times of day. How cool – we now have a data stream of critical neurological data even when the doctor isn’t in. That’s the future of qPLR. Patients and medical professionals working more closely together to help deliver the care the patient needs and outcomes the clinician desires.
The Reflex Team holds weekly Fireside Chats. Subscribe to our YouTube channel to catch the next scheduled Live Fireside Chat held most Tuesdays in the evening (Eastern Time).
Did you like this article? Check out more here: http://18.226.166.241/blog/



Leave A Comment